Osteoporosis in Women: Keeping Your Bones Healthy and Strong
What is osteoporosis?
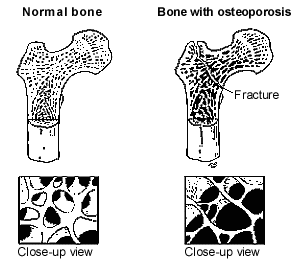
In osteoporosis, the inside of the bones becomes porous from a loss of calcium (see the picture below). This is called losing bone mass. Over time, this weakens the bones and makes them more likely to break.
Osteoporosis is much more common in women than in men. This is because women have less bone mass than men, tend to live longer and take in less calcium, and need the female hormone estrogen to keep their bones strong. If men live long enough, they are also at risk of getting osteoporosis later in life.
Once total bone mass has peaked—around age 35—all adults start to lose it. In women, the rate of bone loss speeds up after menopause, when estrogen levels fall. Since the ovaries make estrogen, faster bone loss may also occur if both ovaries are removed by surgery.
What are the signs of osteoporosis?
You may not know you have osteoporosis until you have serious signs. Signs include broken bones, low back pain or a hunched back. You may also get shorter over time because osteoporosis can cause your vertebrae (the bones in your spine) to collapse. These problems tend to occur after a lot of bone calcium has already been lost.
Am I at risk for osteoporosis?
Risk factors for osteoporosis
| |||
See the box to the right for a list of things that put you at risk for osteoporosis. The more of these that apply to you, the higher your risk is. Talk to your family doctor about your risk factors.
Will I need a bone density test?
Check with your doctor. For many women, osteoporosis (or the risk of it) can be diagnosed without testing. When testing is appropriate, doctors use equipment that takes a “picture” of the bones to see if they are becoming porous.
What about hormone replacement therapy?
Hormone replacement therapy (HRT) is one way to prevent osteoporosis or keep it from getting worse.
In HRT, you take hormones (estrogen and progestin together, or estrogen alone) to counteract the drop in estrogen that happens at menopause or when the ovaries are removed by surgery.
Women who take HRT are at an increased risk for breast cancer, heart attack, stroke, serious blood clots and Alzheimer's disease.
Many physicians now recommend that their patients on HRT stop taking it to prevent osteoporosis.
Factors such as your health history and your family’s health history will be important when weighing the risks and benefits of HRT. Talk to your doctor about whether it’s right for you.
What is calcitonin?
Calcitonin (some brand names: Calcimar, Miacalcin) is a hormone that helps prevent further bone loss and reduces the pain that some people have with osteoporosis.
Calcitonin can be taken as a shot or as a nasal spray. Its most common side effect is nausea.
What are alendronate and risedronate?
Alendronate (brand name: Fosamax) and risedronate (brand name: Actonel) are not hormones, but are used to help prevent and treat osteoporosis. These drugs help reduce the risk of spine fractures by decreasing the rate of bone loss. Their most common side effect is an upset stomach.
What is raloxifene?
Raloxifene (brand name: Evista) is a drug used to prevent and treat osteoporosis by increasing bone density. It is not a hormone, but it mimics some of the effects of estrogen. Side effects may include hot flashes and a risk of blood clots.
What is teriparatide?
Teriparatide (brand name: Forteo) is a new injectable synthetic hormone used once a day for the treatment of osteoporosis. It causes new bone growth. Common side effects may include nausea, dizziness and leg cramps.
How much calcium do I need?
Before menopause, you need about 1,000 mg of calcium per day. After menopause, you need 1,000 mg of calcium per day if you're taking estrogen and 1,500 mg of calcium per day if you're not taking estrogen.
It’s usually best to try to get calcium from food. Nonfat and low-fat dairy products are good sources of calcium. Other sources of calcium include dried beans, sardines and broccoli.
About 300 mg of calcium are in each of the following: 1 cup of milk or yogurt, 2 cups of broccoli, or 6 to 7 sardines.
If you don’t get enough calcium from the food you eat, your doctor may suggest taking a calcium pill. Take it at meal time or with a sip of milk. Vitamin D and lactose (the natural sugar in milk) help your body absorb the calcium.
| ||||